Key Findings
| Highest-Risk States: Rhode Island leads the nation’s worst birth safety states at 80 out of 100 and is the only state with zero rural L&D hospitals. It is joined in the top three by Massachusetts and Connecticut, all three of which have every county classified as a maternity care desert.The New England Paradox: Five of America’s ten highest-risk states are in New England, proving that wealth and healthcare spending alone cannot guarantee maternity care access, with all five having 100% maternity care desert coverage.Safest States: Maryland and Utah are America’s two safest states for expectant mothers, with Maryland scoring just 10.5 out of 100, backed by 78% rural L&D hospital retention and only 4.2% maternity care desert counties. |
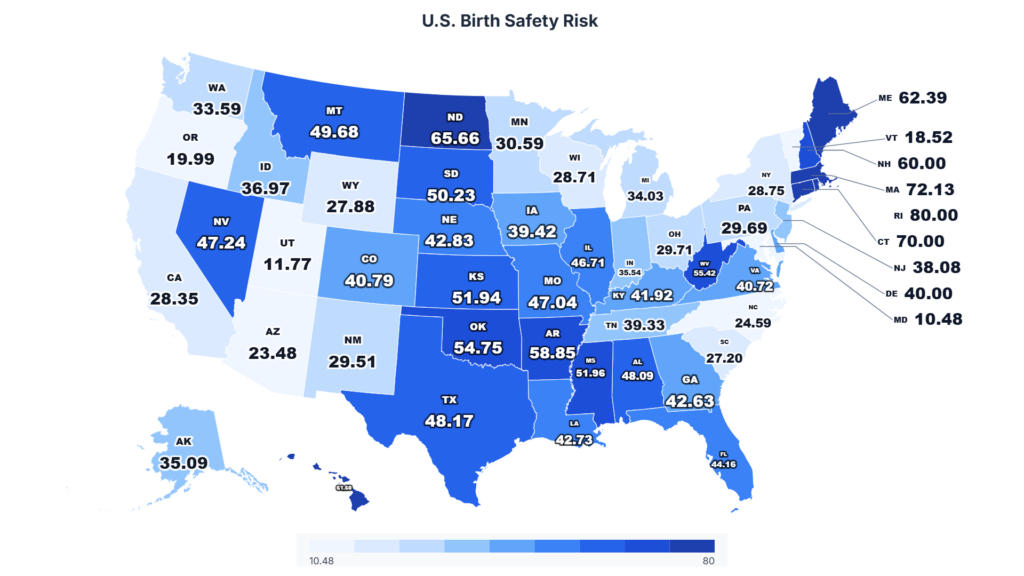
For millions of American women, the closest hospital can no longer deliver their baby. A 50-state analysis reveals that seven states now have every county classified as a maternity care desert, while 54% of rural hospitals nationwide have eliminated labor and delivery services entirely, according to the Center for Healthcare Quality and Payment Reform’s January 2026 Rural Maternity Care Crisis Report.
The study conducted by Birth Injury Lawyers Group analyzed maternity care access across all 50 states using January 2026 data from the Center for Healthcare Quality and Payment Reform and county-level maternity care desert classifications from March of Dimes. States were ranked using a composite Birth Safety Risk score (out of 100) based on three weighted factors: percentage of rural hospitals without L&D services (40 points), closure risk for remaining L&D units (20 points), and percentage of counties classified as maternity care deserts (40 points). Higher scores indicate greater risk.
States With the Highest Birth Safety Risk
Table 1: Top 10 States Ranked by Birth Safety Risk Score in 2026
| Rank | State | Risk Score | % Rural Hospitals Without L&D | % Counties: Maternity Care Deserts | % L&D Units at Risk of Closing |
|---|---|---|---|---|---|
| 1 | Rhode Island | 80.0 | 100% | 100% | 0% |
| 2 | Massachusetts | 72.1 | 43% | 100% | 50% |
| 3 | Connecticut | 70.0 | 25% | 100% | 67% |
| 4 | North Dakota | 65.7 | 82% | 71.7% | 14% |
| 5 | Maine | 62.4 | 50% | 100% | 8% |
| 6 | Hawaii | 61.6 | 54% | 100% | 0% |
| 7 | New Hampshire | 60.0 | 50% | 100% | 0% |
| 8 | Arkansas | 58.9 | 69% | 45.3% | 44% |
| 9 | West Virginia | 55.4 | 79% | 49.1% | 14% |
| 10 | Oklahoma | 54.8 | 71% | 53.2% | 17% |
New England states rank highly due to complete maternity care desert coverage, while Plains, Southern, and Appalachian states suffer from rural hospitals eliminating obstetric services at rates between 69% and 82%.
States With Complete Maternity Care Desert Coverage
Table 2: States Where 100% of Counties Are Classified as Maternity Care Deserts
| State | Risk Score | National Rank | % Rural Hospitals Without L&D | % L&D Units at Risk of Closing |
|---|---|---|---|---|
| Rhode Island | 80.0 | 1 | 100% | 0% |
| Massachusetts | 72.1 | 2 | 43% | 50% |
| Connecticut | 70.0 | 3 | 25% | 67% |
| Maine | 62.4 | 5 | 50% | 8% |
| Hawaii | 61.6 | 6 | 54% | 0% |
| New Hampshire | 60.0 | 7 | 50% | 0% |
| Delaware | 40.0 | 27 | 0% | 0% |
Seven states have every county classified as a maternity care desert, failing to meet minimum maternity care access thresholds statewide, with six of seven ranking in the top half of highest-risk states nationally.
Note: Delaware qualifies for this table solely on the maternity care desert criterion, 100% of its counties are classified as maternity care deserts, despite having 100% of rural hospitals retaining L&D services.
States Facing the Greatest Risk of L&D Unit Closures
Table 3: Top 10 States by Percentage of L&D Units at Risk of Closing
| Rank | State | % L&D Units at Risk of Closing | % Rural Hospitals With L&D | Current Birth Safety Risk Rank |
|---|---|---|---|---|
| 1 | Connecticut | 67% | 75% | 3 |
| 2 | Massachusetts | 50% | 57% | 2 |
| 3 | Arkansas | 44% | 31% | 8 |
| 4 | Kansas | 27% | 36% | 12 |
| 5 | Missouri | 24% | 42% | 18 |
| 6 | Texas | 20% | 41% | 15 |
| 7 | Alabama | 20% | 29% | 16 |
| 8 | Idaho | 20% | 52% | 31 |
| 9 | Oklahoma | 17% | 29% | 10 |
| 10 | New York | 17% | 44% | 40 |
Twenty states face double-digit closure risk for remaining L&D units, with the top three states potentially losing between 44% and 67% of their remaining maternity care infrastructure.
States With the Fewest Rural Hospitals Offering L&D Services
Table 4: Top 10 States by Percentage of Rural Hospitals Without L&D
| Rank | State | % Rural Hospitals With L&D | % Rural Hospitals Without L&D | Risk Score | National Risk Rank |
|---|---|---|---|---|---|
| 1 | Rhode Island | 0% | 100% | 80.0 | 1 |
| 2 | Florida | 9% | 91% | 44.2 | 20 |
| 3 | North Dakota | 18% | 82% | 65.7 | 4 |
| 4 | West Virginia | 21% | 79% | 55.4 | 9 |
| 5 | Illinois | 25% | 75% | 46.7 | 19 |
| 6 | Louisiana | 25% | 75% | 42.7 | 22 |
| 7 | Oklahoma | 29% | 71% | 54.8 | 10 |
| 8 | Alabama | 29% | 71% | 48.1 | 16 |
| 9 | Nevada | 29% | 71% | 47.2 | 17 |
| 10 | Virginia | 29% | 71% | 40.7 | 26 |
In twelve states, fewer than one-third of rural hospitals offer labor and delivery services, potentially requiring pregnant women in these communities to travel farther for childbirth.
States With the Lowest Birth Safety Risk
Table 5: Top 10 Safest States by Birth Safety Risk Score in 2026
| Rank | State | Risk Score | % Rural Hospitals With L&D | % Counties: Maternity Care Deserts | % L&D Units at Risk of Closing |
|---|---|---|---|---|---|
| 50 (Safest) | Maryland | 10.5 | 78% | 4.2% | 0% |
| 49 | Utah | 11.8 | 95% | 20.7% | 5% |
| 48 | Vermont | 18.5 | 69% | 7.1% | 11% |
| 47 | Oregon | 20.0 | 71% | 8.3% | 17% |
| 46 | Arizona | 23.5 | 48% | 6.7% | 0% |
| 45 | North Carolina | 24.6 | 64% | 21.0% | 6% |
| 44 | South Carolina | 27.2 | 45% | 13.0% | 0% |
| 43 | Wyoming | 27.9 | 52% | 21.7% | 0% |
| 42 | California | 28.3 | 42% | 6.9% | 8% |
| 41 | Wisconsin | 28.7 | 51% | 15.3% | 10% |
The safest states demonstrate that preserving rural maternity infrastructure is achievable, with Utah maintaining L&D services at 95% of rural hospitals and Maryland combining strong hospital retention with minimal maternity care desert coverage.
Methodology
The study scored all 50 states on a 100-point Birth Safety Risk index using January 2026 CHQPR and March of Dimes data across three weighted components: rural hospitals without L&D services (40 pts), L&D units at risk of closing (20 pts), and counties classified as maternity care deserts (40 pts). A maternity care desert is a county lacking birthing facilities and adequate obstetric providers. An at-risk L&D unit is defined by CHQPR as a hospital reporting negative financial margins for two or more consecutive years. Higher scores indicate greater risk. Urban access, travel times, birth outcomes, and care quality are not captured.
Data Sources
Rural Maternity Care Crisis Report, January 2026: https://chqpr.org/downloads/Rural_Maternity_Care_Crisis.pdf
Maternity Care Deserts Reports by State: https://www.marchofdimes.org/peristats/reports/alabama/maternity-care-deserts
Research Dataset: https://docs.google.com/spreadsheets/d/1fgyr_zgday730JodEwnLughi7WfvjOH9FA03100iUPY/edit?gid=0#gid=0
Study by: https://birthinjurylawyer.com/
About Birth Injury Lawyers Group
Birth Injury Lawyers Group provides legal representation to families affected by birth injuries across the United States. The firm works with families who have experienced preventable harm during labor, delivery, and the immediate postpartum period. This analysis was conducted to better understand geographic disparities in maternity care access and the systemic conditions that may contribute to adverse birth outcomes nationwide.

